Raising awareness of bowel cancer amidst rising rates
Introduction
In the UK, bowel cancer is the fourth most common cancer, with with over 42,000 people diagnosed every year . When detected early (stage 1), patients have a much higher chance of surviving, at a rate of 9 out of 10. When diagnosed late at stage 4, the survival rate drops to 1 out of 10.
In 2023, the rate in England, from NHS data , was at 73 cases per 100,000 population, and the incidence internationally has been rising sharply over the last 30 years, especially in younger adults.
Several risk factors have been attributed to this global phenomenon, including sedentary lifestyle, coupled with ultra-processed food, leading to obesity. These factors are associated with biological processes that may increase cancer risk, including DNA damage and disruption to normal cell regulation.
Similarly, environmental toxins like micro-plastics and a disturbed gut microbiome (gut bacteria) lead to disruption in the healthy cell replication process and detection of damaged cells.
What private healthcare data shows
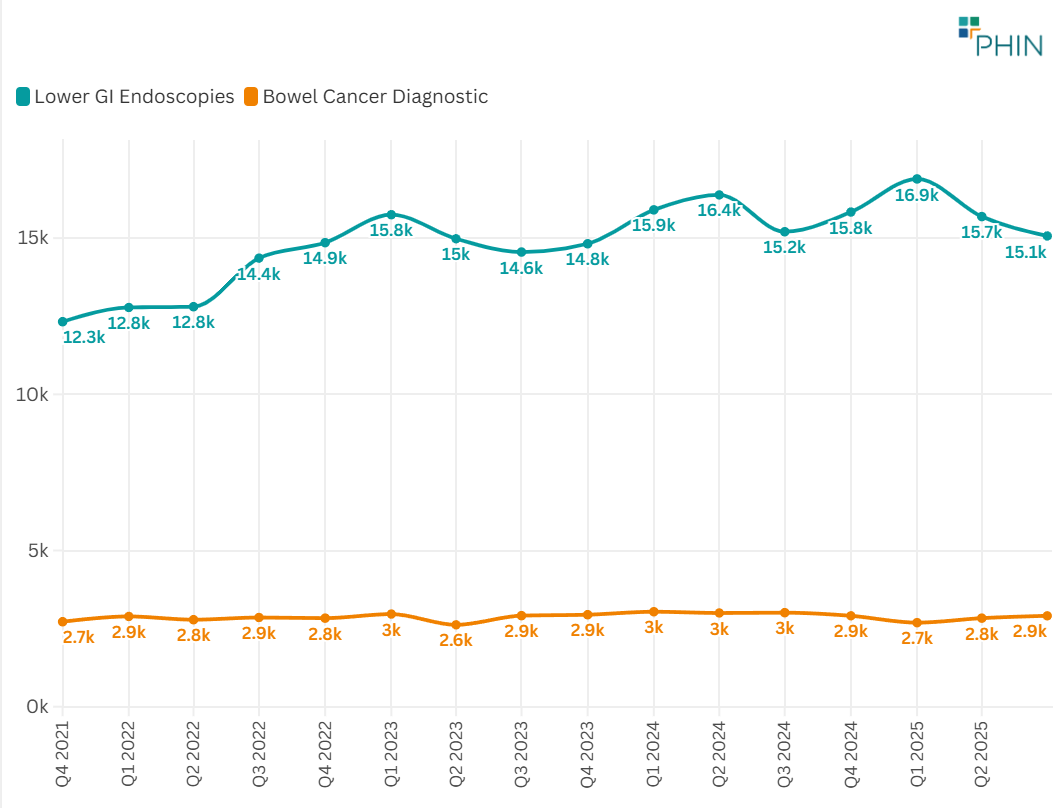
In the UK private sector, there were 46,000 admissions for the management and treatment of bowel cancer over a four-year period. The data indicates an upward trend, with a 7% increase for admissions with bowel cancer as the primary diagnosis between Q4 2021 and Q3 2025, and a 22% increase in admissions for lower gastrointestinal endoscopic procedures (including colonoscopy and sigmoidoscopy) procedures.
Figure 1. Admissions with a diagnosis of Bowel Cancer and lower gastrointestinal endoscopic procedure admissions, UK (Q4 2021–Q3 2025)
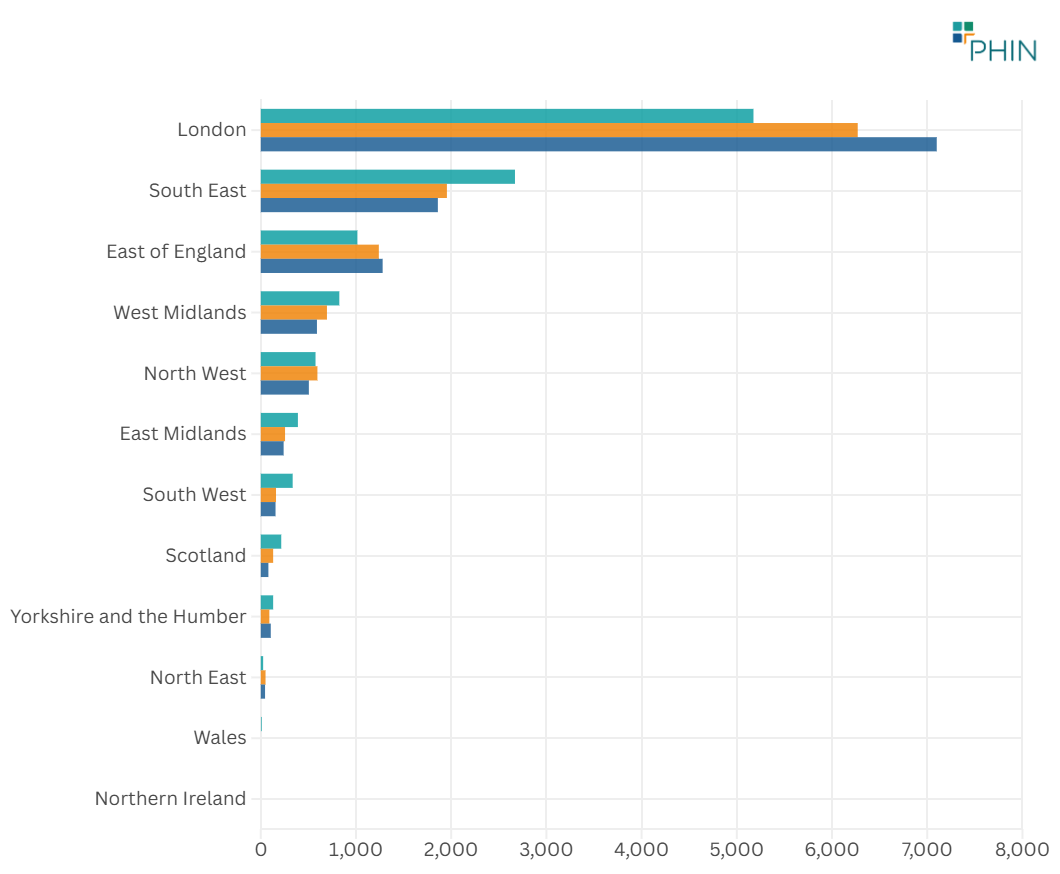
Across the UK, between 2022 and 2024, London consistently recorded the highest admission volumes and the strongest year-on-year growth. This is consistent with London’s role as the largest private healthcare market in the UK.
In contrast, other regions, including the South East, showed a reduction in admission volumes over the same period, with the South East experiencing the largest decrease between 2022 and 2024.
Figure 2. Admissions with a diagnosis of Bowel Cancer by UK nation or English region (2022 to 2024)
| Region | 2022 | 2023 | 2024 |
|---|---|---|---|
| East Midlands | 390 | 260 | 240 |
| East of England | 1,015 | 1,240 | 1,280 |
| London | 5,180 | 6,280 | 7,115 |
| North East | 30 | 50 | 45 |
| North West | 575 | 595 | 505 |
| Northern Ireland | * | * | * |
| Scotland | 215 | 130 | 80 |
| South East | 2,675 | 1,980 | 1,875 |
| South West | 335 | 160 | 155 |
| Wales | 20 | 35 | 65 |
| West Midlands | 825 | 695 | 590 |
| Yorkshire and The Humber | 130 | 90 | 105 |
Early detection is improving, but unevenly
There are, however, encouraging signs and the outlook includes significant positives.
According to The Lancet , rates are plateauing and sometimes even decreasing in some countries for the over-50 population. This can be explained partly due to changes in multiples risk factors, like eating habits and/or physical activity, but also thanks to an increased effort in early detection and diagnosis.
Figure 3. Admissions with a diagnosis of Bowel Cancer by age group (<50 vs =50), UK (Q4 2021–Q3 2025)
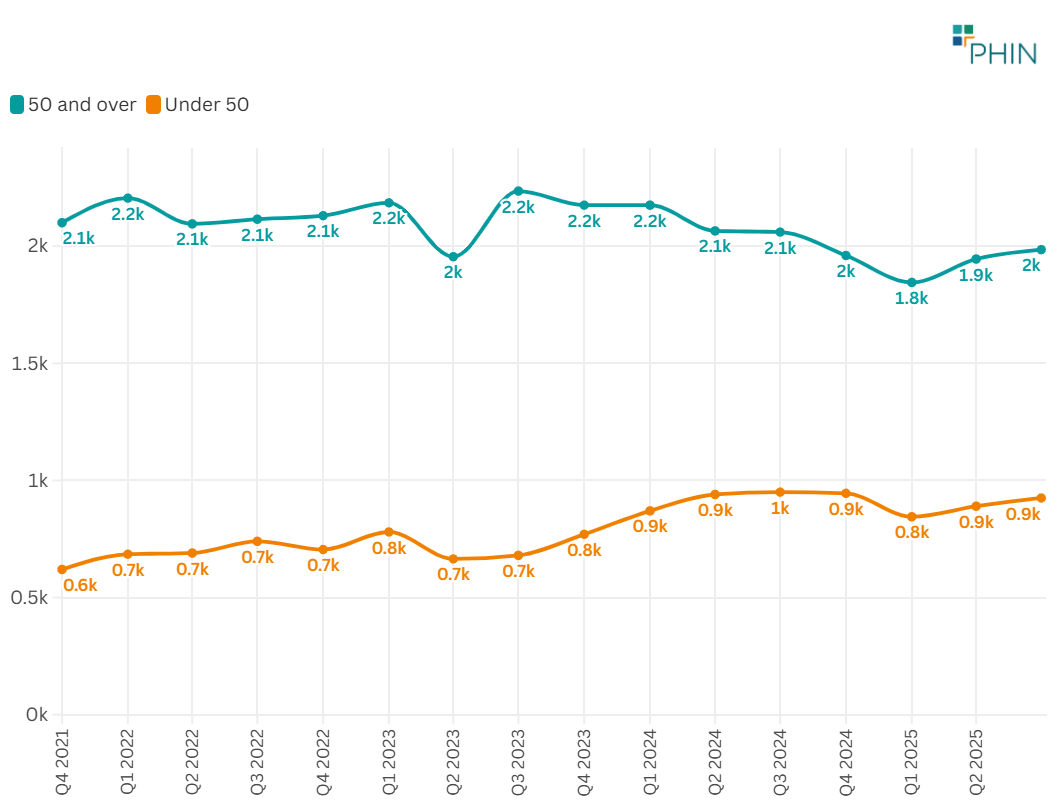
In the private sector, the number of admissions for patients with a confirmed bowel cancer diagnosis in the over-50 group stayed relatively stable, hovering at about 2,000 admissions per quarter [noting a decrease of 6% in Q3 2025 compared to Q4 2021], supporting the claim from the Lancet article .
In contrast, figures for the under-50 group went from 620 in Q4 2021 to 925 in Q3 2025, which represents a 50% increase.
The NHS is certainly committed to the early diagnosis effort and is lowering the threshold of a routine home screening test (FIT – faecal immunochemical test) for the over-50s, that should trigger further investigations, such as endoscopy or colonoscopy, expecting to diagnose 11% more bowel cancer and many other conditions that may lead to it.
For the under-50 population, admissions are increasing at a faster rate, in contrast to the relatively stable trend observed in the over-50 group, there is not yet a plan for routine checks, unless symptoms appear or the patient belongs to a high-risk/hereditary group.
In both age groups, changes to screening thresholds are expected to lead to a higher demand for diagnostic testing, with NHS projections 5 indicating around 35% more endo-colonoscopies.
However, more colonoscopies do not necessarily translate into better outcomes. a study by Professor Eva Morris suggests that for every 10 cases of bowel cancer missed during colonoscopy, around 7 may have been avoidable. This raises the question of whether the NHS can absorb increased demand for colonoscopy without compromising quality.
An opportunity for the independent sector?
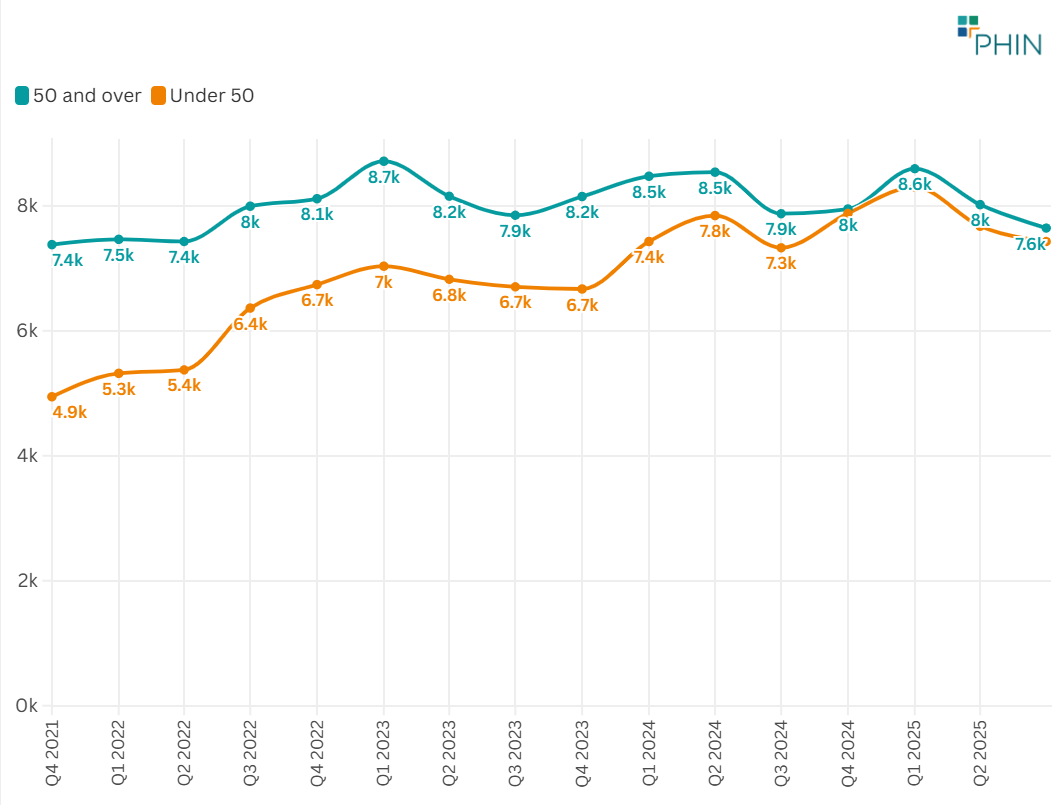
The private sector can certainly help and appears to do so already. With an increase in lower GI endo/colonoscopies of 8% for the over-50 and a 48% increase for the under-50 population since Q4 2021, we clearly see an uptrend and are expecting even more demand once that new lower threshold for FIT screening comes in. The volume of Lower GI procedures for the under-50s overtook the over-50s in Q2 2023 and is now staying above despite quarterly fluctuations.
Figure 4. Lower GI endo-colonoscopy procedure admissions by age group (<50 vs =50), UK (Q4 2021–Q3 2025)
More demand for screening and treatment means more pressure on an already strained NHS capacity. Patients might turn to private providers for earlier diagnosis and the consequent better outcomes. Will the independent sector be ready? What opportunities can be taken?
Conclusion
Bowel cancer incidence is rising internationally, and the UK is seeing similar trends. Early diagnosis and intervention improve survival. New screening protocols will support earlier detection, but only if the supply for diagnostic testing can match the increases in demand. Combined with the increasing use of novel and personalised treatments, the outlook for this condition looks brighter.
While early diagnosis requires increased resources in the short to midterm, the longer-term benefits for patients and the healthcare system are substantial. The analysis highlights increasing demand for bowel cancer diagnostic and treatment services, which will place additional pressure on existing capacity.
Understanding how this demand is distributed across the healthcare system is therefore important when considering how future diagnostic and treatment needs may be met.
These insights highlight the value of independently collected private healthcare data in understanding how diagnostic demand is shifting across the healthcare system.
Disclaimer and caveats
PHIN’s data is drawn from a unique dataset of private admissions submitted by independent hospitals and NHS private patient units (PPUs). PHIN only collects day case and inpatient admissions. Outpatients are not included and some procedures may be underrepresented in this article.
Throughout this article, volumes are shown as admissions (hospital spells) where a bowel cancer diagnosis or a relevant lower gastrointestinal procedure occurred, rather than counts of individual procedures.
Bowel cancer is identified using C18*, C19*, C20* of ICD-10 as primary diagnostic. Lower gastrointestinal endoscopy procedures admissions are calculated based of PHIN’s own OPCS classification system.
